Time Is Muscle
Among her research findings, new Tuck professor Lauren Lu has found a way to reduce 40 minutes of time when transferring heart attack patients between hospitals.

Lu finds that hospitals’ choices of transfer destinations are driven by relationships between hospitals, or sister hospitals, rather than quality or distance—both of which can improve patient outcomes and lead to cost savings.
For new Tuck professor Lauren Lu, a silver lining of 2020 was the ability to focus squarely on her research and utilizing her findings to make a positive impact in the world. During an especially turbulent time in health care, what really strikes a chord with the Daniel T. Revers T’89 Faculty Fellow is the growing issue of health care expenditures and access to quality medical care in the U.S.
“There needs to be better operations and more efficiency in health care systems,” says Lu, who joined Tuck from UNC’s Kenan-Flagler Business School. “People’s lives are at stake here. I saw the potential as a researcher to contribute to saving more lives.”

Tuck professor Lauren Lu is teaching Supply Chain Management at Tuck this spring. Her research investigates the performance of various health care systems with a focus on nursing home operations.
Lately Lu is focused on how health care operations and health information technology can be improved to provide better quality of care and even save lives. Specifically, she is taking a close look at nursing home operations as well as health care delivery for heart attack patients.
We sat down with Lu, who is teaching Supply Chain Management at Tuck this spring, to learn more about her latest research findings and what makes her tick.
Are nursing homes in trouble?
Nursing homes are suffering—there’s no other word to describe it. Even prior to COVID-19, the U.S. nursing home industry was struggling financially, and many nursing homes are running with negative operating margins.
Nursing home operating costs are increasing rapidly as the population is aging. Nursing home residents are typically 85 years or older, have many health complications, and require a signiciant amount of care. And then of course, with COVID-19, costs have increased dramatically.
The industry is facing major challenges and there is no easy solution here. I'm very concerned about the viability of nursing home care over the next 20 years.
What’s one opportunity you see in terms of increasing access to quality nursing home care?
In order to increase public awareness of nursing home quality, the Centers for Medicare and Medicaid Services (CMS) released an online government rating system, Nursing Home Compare. However, the public is largely unaware of the existence of this website and it is also difficult to navigate. As part of a working paper, I am comparing quality ratings on Nursing Home Compare with those on Yelp.com, which consumers are very familiar with. In fact, you can search for thousands of nursing homes on Yelp and read their consumer reviews. What we’ve found is that, Yelp ratings have a much stronger effect on consumer choice of nursing homes than government ratings on Nursing Home Compare.
My research recommends that CMS partner with social media sites like Yelp.com to increase public usage and awareness of Nursing Home Compare.
Well-intentioned laws to improve individual worker performance can have a negative impact on the care quality of nursing homes. Nursing home administrators should work to reduce their reliance on contract nurses.
You also published an impactful paper recently in Management Science focused on mandatory overtime laws for nurses. Tell me more about that research.
You often hear that nurses have to work long hours and suffer from prolonged fatigue. To prevent work-related injuries and to reduce fatigue-related medical mistakes, 16 U.S. states passed laws that prohibit employers from requiring nurses to work overtime. We wanted to know whether these laws improved quality of care in nursing homes.
We found that, while prohibiting mandatory overtime improved job satisfaction among nurses, the overall quality of care provided to residents in nursing homes had decreased. Why? When there were peaks in demand for staff, without the option to use overtime to cover additional staffing needs, management resorted to hiring more contract nurses. These contract nurses work for nurse agencies and are flexible enough to be hired on a daily basis, but they don’t know the residents or their needs. The key message to policy makers is: These well-intentioned laws to improve individual worker performance can have a negative impact on the care quality of nursing homes. Nursing home administrators should work to reduce their reliance on contract nurses.
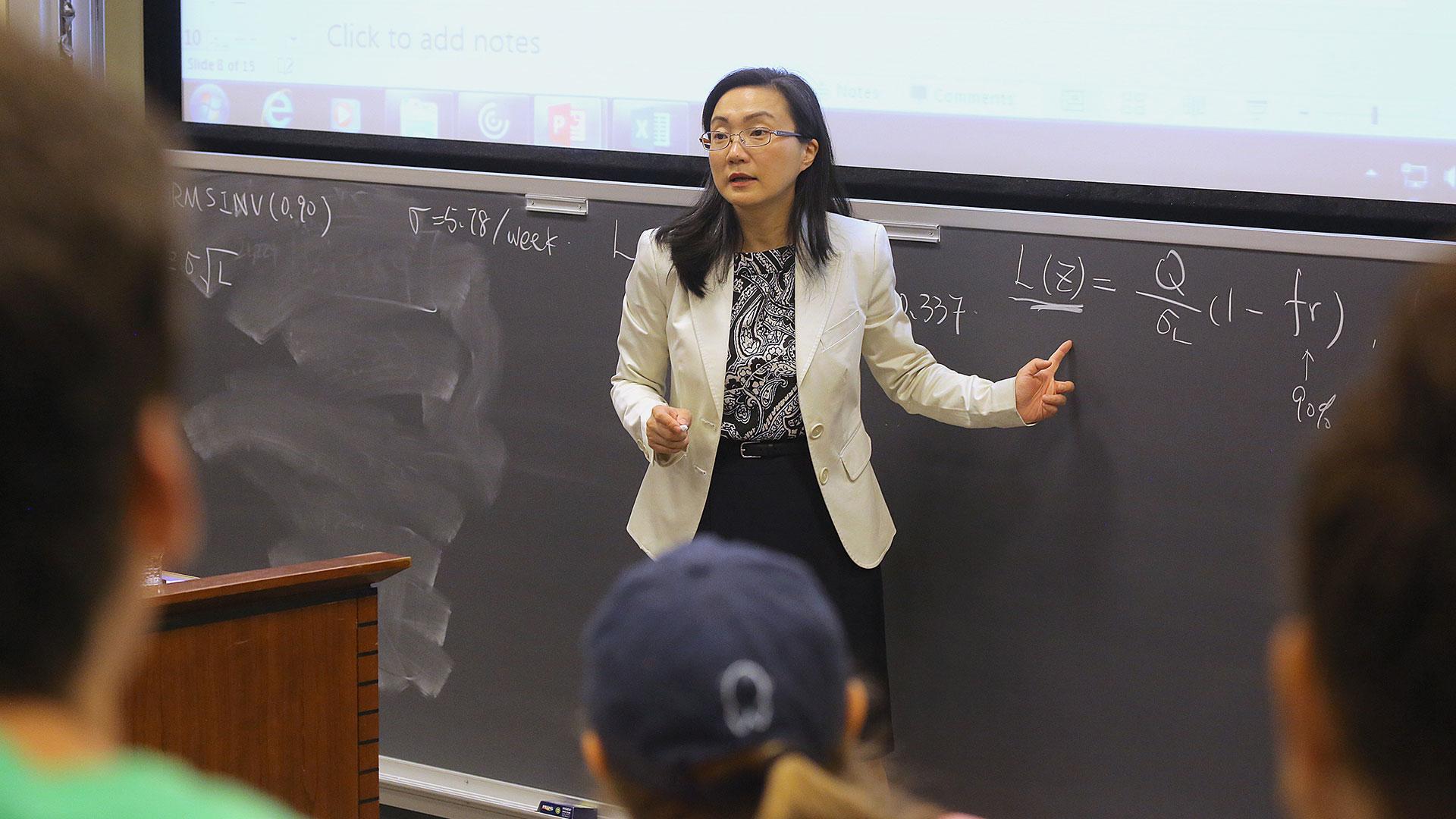
I understand you also conduct research on care delivery for heart attack patients. What led you to pursue this research?
In the U.S., although treatment for heart attack patients has advanced in the last few decades, not everyone has easy access to heart attack care, which is very costly. Two major procedures for heart attack patients are PCI [Percutaneous Coronary Intervention] and CABG [Coronary Artery Bypass Grafting], which many know as open heart surgery. These procedures cannot be performed at your average hospital—you need specialized equipment, experienced cardiologists, and heart surgeons. Rural hospitals do not possess these kinds of resources, so patients need to be immediately transported to a higher level hospital.
I looked into hospital transfer data in Florida, and surprisingly, hospitals’ choices of transfer destinations are driven by relationships between hospitals, or sister hospitals, rather than quality or distance, both of which can improve patient outcomes and lead to cost savings. Hospital administrators should look into their transfer processes and develop transfer policies to ensure best patient outcomes.
And how can better health IT help improve care for heart attack patients?
In the last 10 years, the U.S. government has invested billions of dollars in EHR [Electronic Health Records] systems for U.S. hospitals. Today, over 80 percent of U.S. hospitals have a basic form of EHR. However, this doesn’t mean that these EHR systems of different hospitals easily talk to each other. So when a patient is transferred from hospital A to hospital B, if these two hospitals are not what we call interoperable, then the medical records of the patient cannot be easily accessed by doctors and nurses at the destination hospital.
Time is muscle when we’re talking about cardiac treatment. … If you can save 40 minutes in the transfer process, you might be saving one more life. It’s as serious as that.
We do find, however, that if these two hospitals’ EHR systems are made interoperable, this can translate into a better health outcome for transferred patients. For heart attack patients, we find that hospital transfer time can be reduced by about 40 minutes.
Time is muscle when we’re talking about cardiac treatment. When a patient is experiencing a severe heart attack, every minute that passes by, the muscle in the heart is dying. So if you can save 40 minutes in the transfer process, you might be saving one more life. It’s as serious as that.
This article originally appeared in print in the winter 2021 issue of Tuck Today magazine.

